|
After translating the DHI into Norwegian, the aim of the present study was to examine reliability and validity of the translated version, which was to be used as a descriptive and evaluative measure. Valuable information can be derived in the clinic from tools assessing self-perceived consequences of dizziness, presupposed satisfactory measurement properties. The ability to detect real change in the concept being measured, or the ability to distinguish between participants who have and have not changed an important amount, have not been reported. The ability of the DHI to measure meaningful or clinically important change, has scarcely been examined, and variable results regarding the ability of the DHI to discriminate between treatment and control groups, have been found in randomized controlled trials. Satisfactory test-retest reliability has been demonstrated for the total scale as well as for the subscales, and a change in the DHI total score should decrease by at least 18-points in individual patients to be called a true change. Concurrent validity has been examined in several studies, presenting variable results. Validity of the DHI was indicated as higher scores were associated with higher frequency of dizziness and with greater functional impairments. High internal consistency has been demonstrated for the total scale as well as for the subscales. Later studies of the underlying factor structure of the DHI failed to support the empirically developed sub-domains, which was also adressed in a recent review article. The scale was developed to capture various sub-domains of self-perceived handicap and comprises 7 physical, 9 functional, and 9 emotional questions. The DHI contains 25 items, and a total score (0-100 points) is obtained by summing ordinal scale responses, higher scores indicating more severe handicap. Items included in the DHI were originally derived from case histories of patients with dizziness, and the measure was further examined in several studies involving patients seen for vestibulometric testing. Translation of the DHI has also been demanded by clinicians and researchers in Norway. The original American version has been translated and adapted to several languages and cultures, like Swedish, Chinese, and Dutch. 
The self-report questionnaire was originally designed to quantify the handicapping effect of dizziness imposed by vestibular system disease, but has also been used for persons with dizziness of other origins. The Dizziness Handicap Inventory (DHI) is used in clinical work and in research to assess the impact of dizziness on quality of life. This is the first study that has addressed and demonstrated responsiveness to important change of the DHI, and provided values of SDD and MIC to help interpret change scores. The DHI-N total scale demonstrated satisfactory measurement properties. The MIC was identified as 11 DHI-N points. Responsiveness of the DHI-N was excellent, AUC = 0.83, discriminating between self-perceived 'improved' versus 'unchanged' participants. Correlations between change scores of DHI-N and other self-report measures of functional health and symptoms were high (r = 0.50 - 0.57). Satisfactory test-retest reliability was demonstrated, and the change for an individual should be ≥ 20 DHI-N points to exceed measurement error (SDD). The DHI-N demonstrated excellent ability to discriminate between participants with and without 'disability', AUC being 0.89 and best cut-off point = 29 points. Concurrent correlations between the DHI-N and other related measures were moderate to high, highest with Vertigo Symptom Scale-short form-Norwegian version (r = 0.69), and lowest with preferred gait (r = - 0.36). Acceptable internal consistency was found for the total scale (α = 0.95). Resultsįactor analysis revealed a different factor structure than the original DHI, resulting in dismissal of subscale scores in the DHI-N. Longitudinal designs were used to examine test-retest reliability (intraclass correlation coefficient (ICC) statistics, smallest detectable difference (SDD)), and responsiveness (Pearson's product moment correlation, ROC curve analysis area under the ROC curve (AUC), and minimally important change (MIC)). A cross-sectional design was used to examine the factor structure (exploratory factor analysis), internal consistency (Cronbach's α), concurrent validity (Pearson's product moment correlation r), and discriminate ability (ROC curve analysis). 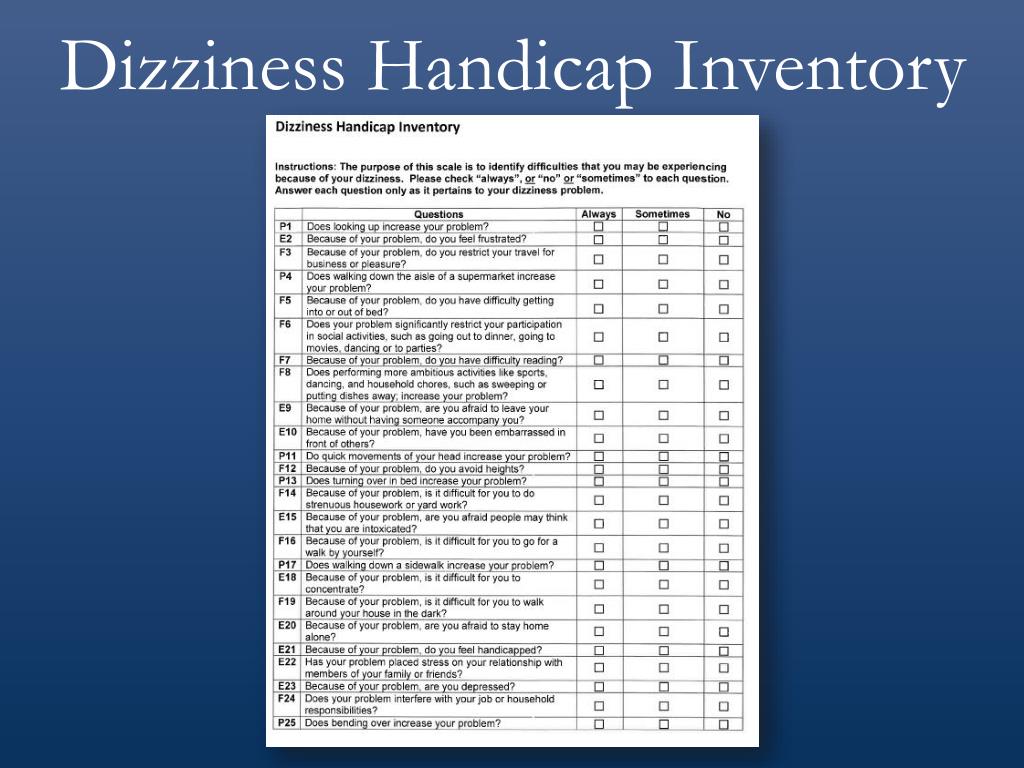 
Two samples (n = 92 and n = 27) included participants with dizziness of mainly vestibular origin. The aim of the present study was to examine reliability and validity of a translated Norwegian version (DHI-N), also examining responsiveness to important change in the construct being measured. The impact of dizziness on quality of life is often assessed by the Dizziness Handicap Inventory (DHI), which is used as a discriminate and evaluative measure.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
